Why and How does "Prone-Sleeping"
concern with Sudden Infant Death
Syndrome(SIDS)?
Shiro Kubota, MD
Masatoshi Sano, MD
Kubota Maternity Clinic
Hirao-2-12-18, Chuoku, Fukuoka,
Japan 810-0014
Phone: 092-531-7530, Fax: 092-531-9840
|
|
| After the "Back-to
Sleep" campaign, the incidence of SIDS
has remarkably decreased in the world1.2.3. However, it has been still unknown why
an infant sleep at supine-position is safer
against SIDS than at prone-position, and
how an infant dies with SIDS. By the observations
of central(C-) and peripheral(P-) deep-body
temperature(DBT) of the infants who slept
in supine and in prone-position, we clarified
that the infants in prone-sleeping get heat-stroke
by the disturbance of thermolysis from abdomen,
when they are put on clothes excessively.
When the cold stimulation is lost continuously,
the warming makes an infant sleep more deeply
and reduces arousal response and respiration,
as a result, hypoxemia of the infant advanced.
It is strongly assumed that SIDS is not a
desease, but is the irreversible stage of
hypoxemia caused by the infant's thermoregulation
during sleep in warm condition. To prevent
from SIDS and to liberate mothers from nursing
apprehensions, it is very important to know
the reasons why infants are sensitive to
heat and to understand the intrinsic and
extrinsic problems surrounding them. |
| Å@As there are many descriptions about the
epidemiological surveys and the autopsy findings
of SIDS which relate to body and environmental
temperetures of infants, it is suggest that
the characteristics of this syndrome may
have relevance to the thermoregulation of
infants. The relationship between SIDS and
over-heating had been mentioned in1970's4.5.6. However, negative relevances between SIDS
and hyperthermia had been recognized in 1980's.
In those days it was difficult to differ
scientifically between fever and heat-stroke
in the infants with hyperthermia. Fever is
usually accompanied with infections. In the
case of an infection, thermoregulation of
the patient corresponds to the person who
regulates the body temperature at low-temperature
environment, because thermoregulation-center
is set erroneously at a high level by pyrogens.
Therefore, thermogenesis is promoted by muscular
strain like shiverings, but thermolysis is
inhibited by peripheral vasoconstriction.
As a result, hands and feet become cooler
and do not sweat. Sweating is generally noted
when the patient begin to recover and peripheral
vessels are dilated. Different from fever,
heat-stroke is generally caused by the the
disturbance of thermolysis and/or the increase
thermogenesis. In the infants, however, the
thermolysis is declined under the environmental
conditions of high temperature and humidity.
It will be easy to make infant over-heating,
because he cannot say a word, cannot turn
over by himself, or cannot remove (bed)clothes
by himself. Under such conditions, his peripheral
blood vesseles are dilated, the hands and
feet are warm, his skin is moist and sweat,
that is, the P- DBT is elevated. |
| The deep-body thermometers using
in this experiments is reported to measure
the DBT at the depth of 9 mm from surface7. One was attached on the sternum and measured
the temperature of the blood in the heart
and the other on the foot sole measured the
DBT at the same part which was correlated
with the peripheral blood flows8. Fig.
1 shows one of the representative records
of them. In the supine-position, the C-DBT
and back-environmental temperature(B-ET)
were higher than the P-DBT and abdominal-ET(A-ET).
The B-ET was equal to C-DBT. After changing
the position from "supine" to "prone",
three temperatures altered as follows. The
A-ET and B-ET rapidly altered within a few
minutes. The A-ET elevated higher than the
C-DBT while the B-ET was declined. B-ET in
the prone position was lower than A-ET in
supine position. On the other hand, the P-DBT
gradually elevated interestingly to reach
in equilibrium about 1 hour later. The C-DBT
showed little variations throughout the observation. |
|
| Figure 1 |
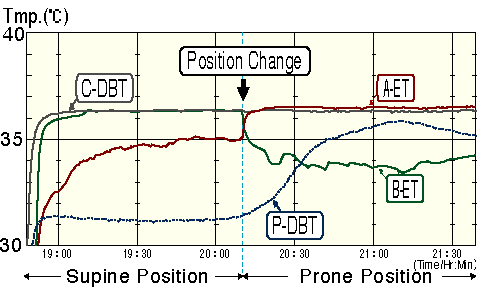 |
Fig.1 The alternations of body temperatures
by changing positions.
The body temperatures of an infant weighed
2,620 grams at the second day after full-term
deliverty was recorded by two deep-body thermometers(Terumo
Co.:PD-3) continuously and simultaneously
. The environmental temperatures (exactly,
between the inner and the outer clothes)
at both the abdomen(A-ET) and the back(B-ET)
were also recorded. The abbreviations in
this figure are as follows, C-DBT: central
deep-body temperature, P-DBP: peripheral
deep-body temperature, A-ET; abdominal environmantal
temperature, B-ET: back environmental temperature.
The obserbations were performed under the
superintendence of one or more doctors and
nurses. Mothers of all infants on this studies
were informed and consented previously. |
|
|
| From the alternations of A-ET
and B-ET by their position change, it was
recognized that the heat of infants is released
much more from their abdomnen than from their
back. The more important phenomena was observed.
The P-DBT gradually rose with the prone-position
as compared with that of the supine-position.
The elevation of P-DBT means as follows.
The vesseles of extremities are dilated to
carry inner heat to outside. Accordingly,
it means that the thermolysis is suppressed
at the prone-position compared with supine-position.
If an infant in prone-position is covered
excessively and insides of clothes become
hot and humid, the heat of the infant
will not be released and be accumulated.
Presumably, it is possible that the P-DBT
of the infant in prone-position and excessive-clothes
reach equilibrium to C-DBT within a few ten
minutes, which will cause "heat-stroke".
The high temperature and humidity of environment
do not mean only the high temperature and
humidity in their room, but also mean those
of the inside of clothes. Caps and
socks also disturb their thermolysis at prone-position.
The homeothermal animals produce heat as
long as they live. If one of them breathe
it last, it did not produce heat any more.
Then, its body temperature become to be variable
by ET. When the ET is high, its body temperature
is still high. This might be the reason why
the body temperature of an infant who died
with SIDS was high. |
|
| Figure 2 |
|
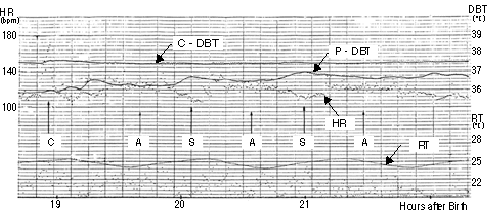 |
| Fig.2 The thermoregulation of an infant at
normal environmental temperature. |
| The deep-doby temperatures were monitored
continuously and simultaneously on a full
term delivery infant in the supine-position,
and the alternation of the heart rate and
his behaviers(awakening or sleeping) were
observed in room temperature(25Åé). The abbreviations
in this figure are as follows, C; crying,
A; awakening, S; sleeping, HR; heart rate,
RT; room temperature. Other abbreviations
are same as Fig.1. |
|
|
| In the cool environment8, to keep their C-DBT normal, infants reduce
the thermolysis by the peripheral vasoconstriction
and produce heat by muscular movements, like
crying. In the normal environment(Fig.2),
C-DBT shows little fluctuations, but P-DBT
altered by the changes of peripheral vasoconstriction
and vasodilatation. The decline of P-DBT
is associated with vasoconstriction, the
increase heart rate and awakening, while
the elevation of P-DBT is associated with
vasodilatation, unfructuated heart rate and
sleeping, respectively. Therefore, it is
assumed that the thermoregulation of the
infants is controlled by the ON/OFF switch
of stimulation via neurotransmitter secretion.
In high temperature environment, however,
infants must continue to release heat by
peripheral vasodilatation, sweat and stop
to produce heat by relaxing muscles. In cool
environment, the cold stimulation makes infants
arousal response and respiratory acceleration.
But in high temperature environment, infants
sleep well and do not receive any cold stimulation.
If over-heating continues for a long time
and the switch of the stimulations continues
to be OFF, an infant will sleep more deeply
and relax the muscles more than usual, as
a result, his/her respiration is more inhibited
and hypoxemia is advanced. It was also observed9 that heart rate of sleeping infants in warm
condition(34Åé) showed little fluctuations
and TcPO2 in warm condition was lower than
those of the infants at room-temperature(25Åé).
Furthermore, in high environmental temperature,
his/her oxygen consumption also increases.
If the neurotransmitter-secretions is continuously
reduced, it is easy to understand that his/her
hypoxemia will be more advanced and will
not be recovered any more. Therefore, it
might be considered that SIDS will happen
when an infant is sleeping deeply without
arousal response and his/her hypoxemia become
irreversible. |
Å@Although there have been at least hundreds
of thousands of victims during the last century,
no one sees the moment of SIDS. The infants
areusually asleep after feeding at night
or in the busy day-care center. If someone
watches the sleeping sick infant by heat-stroke
and the person touches him/her, this touch
stimulation makes him/her arousal and respiration
reactions which let him/her escape from SIDS.
This might be the reason why SIDS has no
eyewitness. Nevertheless, the cold stimulation
exists at night and in the day-care center
as long as the sleeping infants are not covered
excessively, even though there are little
stimulation or no eyewitness. Therefore,
the cold stimulation is the matter of great
importance for the infants to prevent from
SIDS. From our experiments, it was highly
suggested that the cold stimulation disappear
not only by the heating but also by the warming
with excessive clothes. Because, wrapping
an infant keeps away the cold stimulation
from him/her by the high temperature and
humid environment of the inside of clothes.
Consequently, the P-DBT elevates continuously
without rhythmical up-and-down fructuations.
This is the most dangerous for sleeping infants.
If you watch carefully his/her behavior,
it is possible to know whether the environmental
temperature is suitable for him/her or not.
Because the behavior of infants represents
their present conditions. If he/she cries
drawing his/her extremites, he/she
feels cold or uncomfortable. If he/she is
asleep without sweat or warm hands
and feet, he/she might be comfortable. However,
if he/she sleeps deeply with
sweat and warm hands and feet, he/she might
be too warm. It is much better to think that
infants are sensitive to "warmth"
rather than "coolness". Never over-wrap
him/her with the clothes, especially made
of unventilated or bad hygroscopic materials. |
|
References
| 1. |
Wigfield, RE., et al. Can the fall in Avon's
sudden infant death rate be explained by changes
in sleeping position. Br Med J 304, 282-283
(1992) |
| 2. |
Ponsonby, AL., et al. Factors potenciating
the risk of sudden infant death syndrome
associated with the prone position.
N Engl J Med 329, 377-382 (1993) |
| 3. |
Willinger, M., Hoffman, H. & Hartford,
RB. Infant sleep position and risk for sudden infant
death syndrome: Report of meetng held January
13 and 14,1994,National Institute of Health,
Bethesda, MD. Pediatrics 93, 814-819 (1994) |
| 4. |
Dallas, RJ. Cot deaths. Br Med J 3, 347-348
(1974). |
| 5. |
Bacon, C., Scott, D. & Jones, P. Heatstroke
in well-wrapped infants. Lancet i,
422-425 (1979). |
| 6. |
Stanton, AN,, Scott, DJ. & Dowmnham,
MAPS. Is overheating a factor in some unexpected
infant deaths? Lancet i, 1054-1057
(1980). |
| 7. |
Togawa, T., Nemoto, T., Yamazaki, T. &
Kobayashi, T. A modified internal temperature
measurement device. Med Biol Eng 14,
361-364 (1976). |
| 8. |
Kubota, S., et al. Homeothermal ajustment
in the immediate postdelivered infant monitored
by continuous and simultaneous measurement
of core and peripheral body temperatures.
Biol Neonate 54, 79-85 (1988). |
| 9. |
Kubota, S., et al. The alternations of the
temperatures of neonates.Obstet Gynecol Ther(in
JPN) 39, 463-469 (1979). |
|
|
| Acknowledgement |
| We are grateful to Prof. Keiko
Shimizu helped English translation. |
| (June 7,2001) |
|
 Å@Å@Å@ Å@Å@Å@ Å@Å@Å@ Å@Å@Å@ |
|